Search results
10 results found.
10 results found.
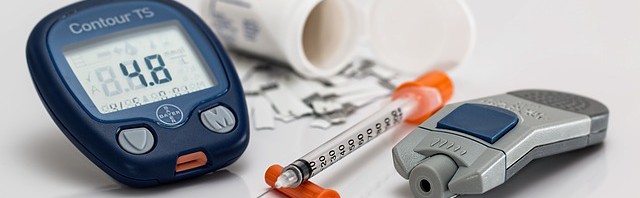
More and more communities across the country are encountering a commonly overlooked public health and safety issue: improper needle and sharps disposal. “Sharps” is a medical term for devices with sharps points or edges that can puncture or cut skin. Examples of sharps are needles, syringes, lancets, auto injectors, epinephrine and insulin pens, infusion sets, and connection needles/sets. The group of people who are put in the most danger by improper sharps disposal are environmental service workers – janitors, housekeepers, waste and recycling workers and sewage treatment workers. When a needle is tossed directly into the trash, it has the […]
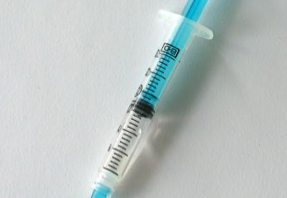
NeedyMeds is pleased to announce our latest partnership with SafeNeedleDisposal.org! In honor of this new partnership we are spotlighting this week’s blog post on the safe disposal of needles. Needle disposal is a public health and safety issue that is commonly overlooked. The problem is that there are limited options for safe disposal of needles which leads to dangerous situations for the public – including injury and the spread of infectious disease. Additionally, information about safely disposing of syringes and needles is difficult to come by and often misunderstood. Each year “approximately 9 million syringe users will administer at […]

Poisoning is the number one cause of injury-related death in the U.S.. National Poison Prevention Week, sponsored by the National Poisoning Prevention Council during the third week in March, promotes poison prevention tips and the free emergency services provided by poison control centers, including the Poison Help hotline at 1-800-222-1222. Text POISON to 797979 to save the number in your smartphone. In the time it takes to read the information above, at least two people will call a poison control center. That’s one person every 14 seconds, according to the American Association of Poison Control Centers’ National Poison Data System […]

Note: This is a rough transcript of episode 14 of Health Savings News and has been lightly edited for clarity. Copy may not be in its final form. [Fundraising appeal] [intro music] (2:09) Evan (2:19): Hello, and welcome to Health Savings News: the podcast about healthcare costs in America and how to save money on the often expensive care all kinds of people need. I’m your host, Evan O’Connor, joined by retired doctors, Rich Sagall and Mike Woods. Each episode we discuss healthcare costs in America, offer tips for saving money, and relevant news that affects and […]

Since our last update on the costs associated with COVID-19 in May, new variants have swept across the country, booster shots have been recommended for most vaccine recipients, and inoculations have been approved for children as young as 5 years old. Americans are still struggling from unexpected pandemic-related healthcare costs. Major systemic failures to meaningfully address the coronavirus pandemic throughout 2020 had dire consequences that the nation and the world are still recovering from. The U.S. contains only 4% of the world’s population, but 20% of global cases and deaths from the pandemic. As many as 40% of American […]